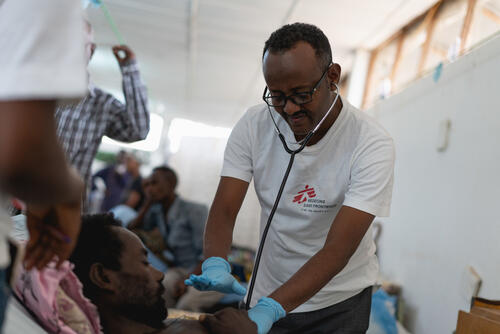
Kala azar
Kala azar is one of the most dangerous neglected tropical diseases (NTDs), and is fatal in 95 percent of cases if left untreated.
Also known as visceral leishmaniasis, kala azar is the most serious form of leishmaniasis and as of 2020 is endemic in 90 countries.
The parasite is spread to humans by bites from infected female sandflies. It attacks the immune system and is almost always fatal if not treated.
It's estimated that there are between 50,000 and 90,000 new cases a year, about 90 percent of which occur in Brazil, Ethiopia, India, Kenya, Somalia, South Sudan and Sudan.
Between 1989 and 2020, MSF treated 150,000 people for kala azar – over a third of them in South Sudan.
Key facts: Kala Azar
90,000
NEW CASES EACH YEAR
95%
FATALITY RATE IF LEFT UNTREATED
150,000
PEOPLE TREATED BY MSF FOR KALA AZAR BETWEEN 1989 AND 2020
What causes kala azar?
Kala azar is caused by bites from female phlebotomine sandflies – the vector (or transmitter) of the leishmania parasite.
The sandflies feed on animals and humans for blood, which they need for developing their eggs.
If blood containing leishmania parasites is drawn from an animal or human, the next person to receive a bite will then become infected and develop leishmaniasis.
Months after this initial infection, the disease can progress into a more severe form, called visceral leishmaniasis or, kala azar.
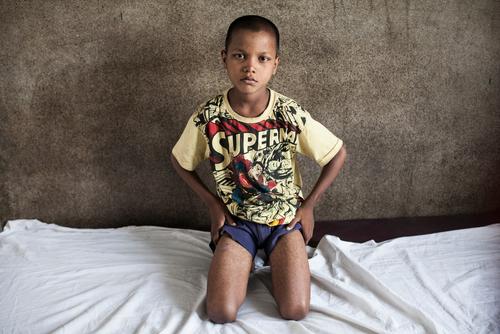
What are the symptoms of kala azar?
Initially, Leishmania parasites cause skin sores or ulcers at the site of sandfly bites. If the disease progresses, it attacks the immune system.
Kala azar presents after two to eight months, with more generalised symptoms, including prolonged fever and weakness.
Co-infection of kala azar and HIV is a major challenge, as the diseases influence each other in a vicious spiral as they attack and weaken the immune system.
How is kala azar diagnosed?
The most effective diagnostic tests for leishmaniasis are invasive and potentially dangerous, where tissue samples are required from the spleen, lymph nodes or bone marrow.
These tests require lab facilities and specialists not readily available in resource-poor, endemic areas.
The most common method of diagnosing kala azar is by dipstick testing. However, this method is highly problematic. In endemic areas, people can become infected with kala azar, but it may not develop into the disease. Therefore, no treatment will be required.
Unfortunately, dipstick testing only establishes whether a patient is immune to kala azar – so if the parasite is present, it would appear that the patient has the disease. Because of this, dipstick testing can’t be used to see if the patient is cured, is re-infected or has relapsed.
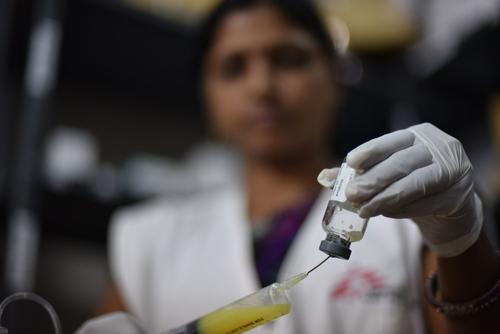
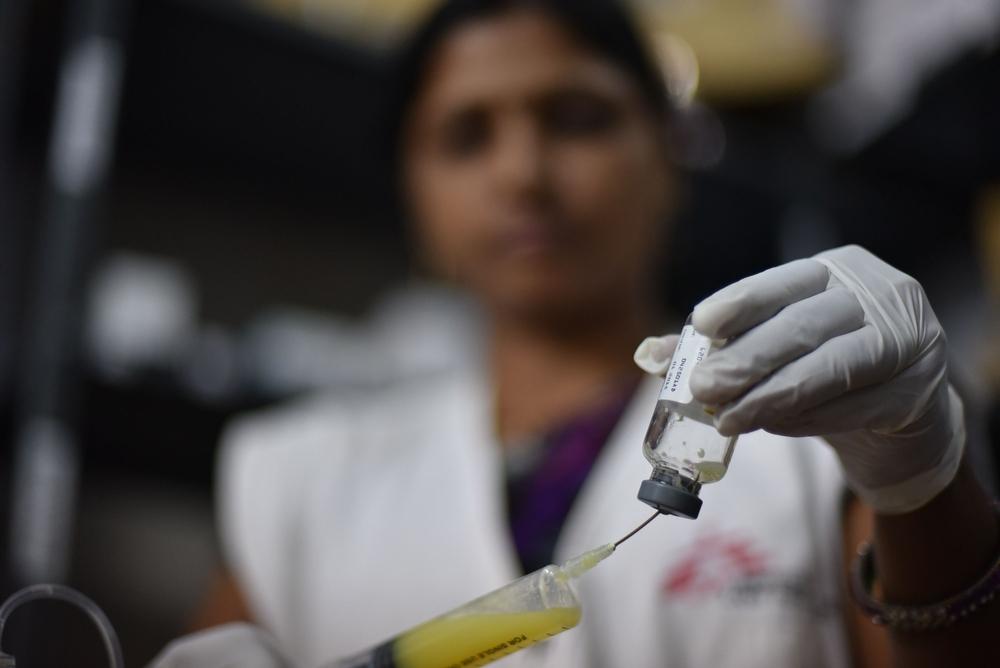
How is kala azar treated?
Today, liposomal amphotericin B is becoming the primary treatment drug in Asia, either alone or as part of a combination therapy.
While safer and shorter than previously used medication, it requires intravenous administration, which remains an obstacle to its use in local clinics. An oral drug, miltefosine, is often added to optimise treatment regimens in patients.
In Africa, the best available treatment is still a combination of pentavalent antimonials and paromomycin, which is toxic and requires a number of painful injections. Research into other treatment combinations is underway.
In 2022, research conducted by MSF and partners in India contributed towards the WHO releasing updated treatment recommendations for people with both HIV and kala azar.
Spotlight: Kala azar in Bihar, India
Kala azar: News and stories