Sorry, that story no longer exists on our website
The article or video you are looking for has been moved to our archive. Perhaps another story on this page might interest you?
Scroll down for links to our latest news, crisis explainers and videos from our projects.
Latest news and stories from MSF UK

All you need to know about the Bundibugyo virus which is causing the current Ebola disease outbreak
Learn more

Escalating violence in South Sudan has left an estimated 762,000 people without access to healthcare
Learn more

In the Democratic Republic of Congo, MSF teams are mobilising to help contain the sudden surge in Ebola cases
Learn more
Never miss another story
Sign up to Frontline, our monthly e-newsletter, to stay up to date with MSF's life-saving work in over 65 countries
MSF crisis responses explained
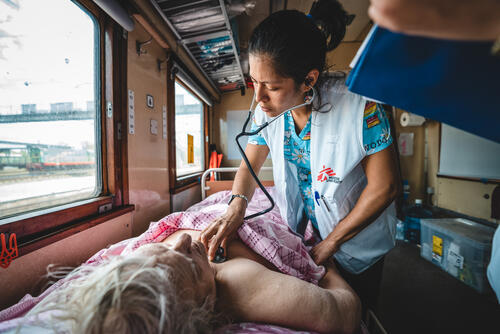
From the first days of the crisis, MSF has worked to deliver medical aid to people in Ukraine
Learn more

Yemen is in the middle of a complex humanitarian crisis driven by a brutal civil war
Learn more









