Sorry, that story no longer exists on our website
The article or video you are looking for has been moved to our archive. Perhaps another story on this page might interest you?
Scroll down for links to our latest news, crisis explainers and videos from our projects.
Latest news and stories from MSF UK

Israel's use of starvation as a weapon in Gaza has reached unprecedented levels, as patients and healthcare workers themselves struggle to survive
Learn more
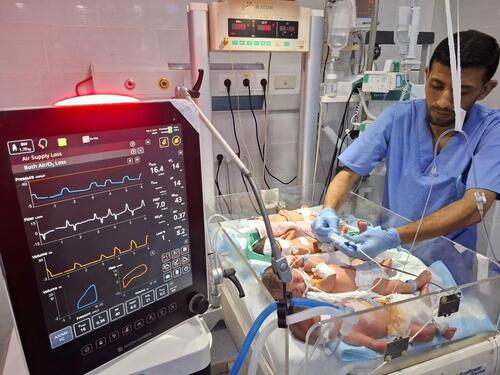
Medical teams in Gaza lack essential equipment such as ultrasounds, incubators, medical supplies, and even baby formula, to keep premature babies alive
Learn more

MSF joins more than 100 organisations to sound the alarm on famine in Gaza and call for life-saving aid
Learn more
Never miss another story
Sign up to Frontline, our monthly e-newsletter, to stay up to date with MSF's life-saving work in over 65 countries
MSF crisis responses explained
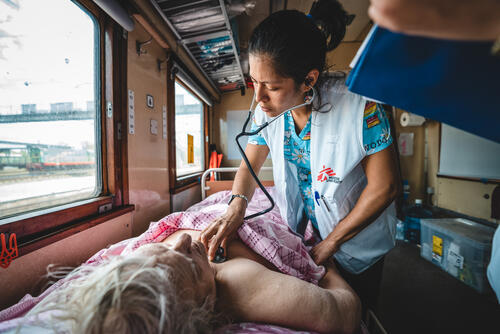
From the first days of the crisis, MSF has worked to deliver medical aid to people in Ukraine
Learn more

Yemen is in the middle of a complex humanitarian crisis driven by a brutal civil war
Learn more